
Book a Consultation
Thank you!
Your form has been sent successfully.



September 05, 2023
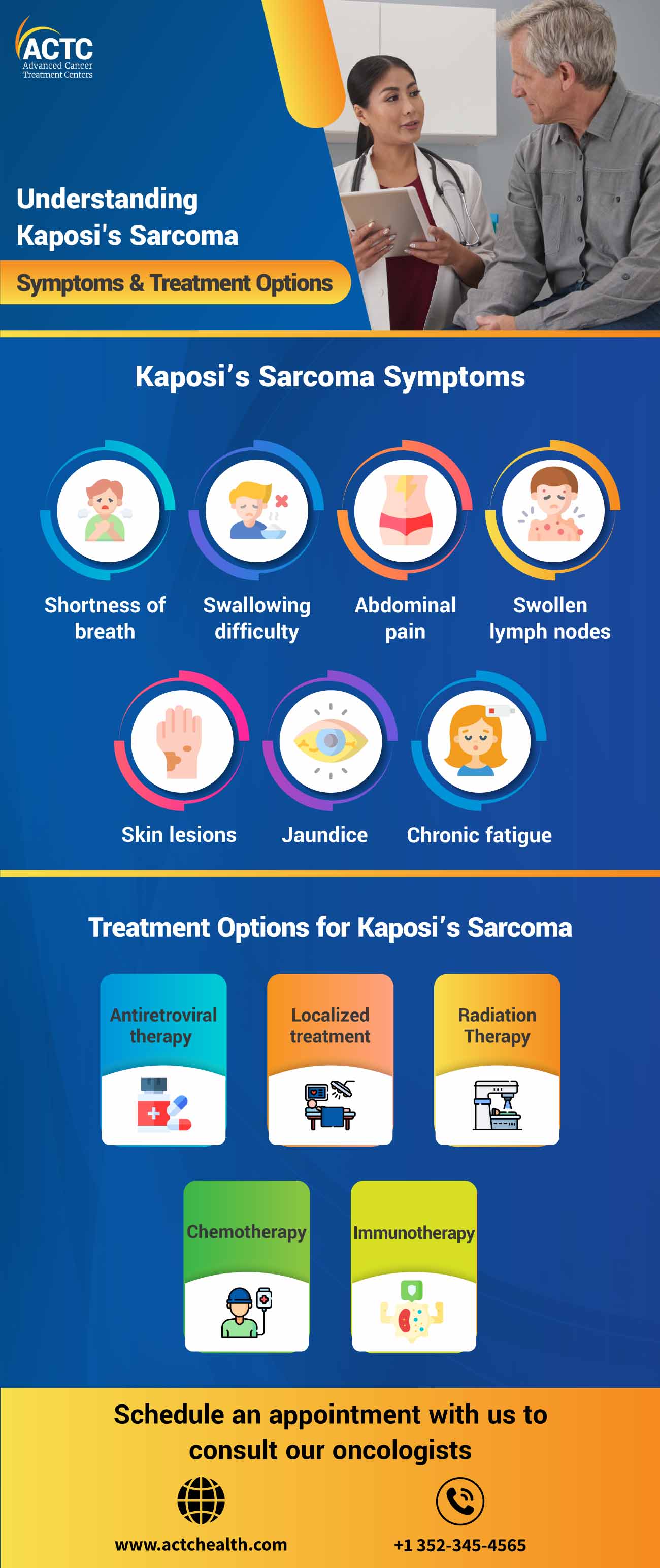
Kaposi's Sarcoma is a rare form of cancer that primarily affects the skin, but can also involve other organs like the mouth, lymph nodes, and internal organs. Researchers have been studying this disease since the early 1980s when the HIV and AIDS epidemic came into the spotlight. This form of cancer is usually caused by Human Herpesvirus 8 (HHV-8) infection and immunodeficiency.
In this comprehensive blog post, we will share Kaposi's sarcoma symptoms, its types, and treatment options. Read on to learn more.
This cancer can manifest in the following forms, each with unique characteristics and underlying causes.
It is the rarest form of the disease, primarily affecting older adults. Classic Kaposi’s is a slow-growing cancer, often limited to the skin and producing red, purple, or brown lesions on the lower extremities. Unlike other types of Kaposi's sarcoma, this is less commonly associated with HIV or immunosuppression.
It is prevalent in certain regions of Africa, especially sub-Saharan Africa, primarily affecting young adults and children. It is more aggressive than the classic Kaposi’s and can involve the lymph nodes, and internal organs along with the skin. Endemic Kaposi's Sarcoma is associated with the infection caused by the Human Herpesvirus 8 (HHV-8).
The epidemic form of Kaposi's Sarcoma gained significant attention during the HIV/AIDS pandemic, and it remains a significant concern in individuals living with HIV. The weakened immune system resulting from HIV infection allows HHV-8 to replicate, leading to the development of numerous lesions on the skin, mucous membranes, lymph nodes, and internal organs.
It occurs as a result of immunosuppressive therapy given to organ transplant recipients or individuals with certain autoimmune diseases. The immunosuppressive drugs, while necessary for preventing organ rejection or controlling autoimmune conditions, can also reactivate HHV-8, leading to the development of Kaposi's Sarcoma. This form of the disease may resemble the epidemic type and affect various organs.
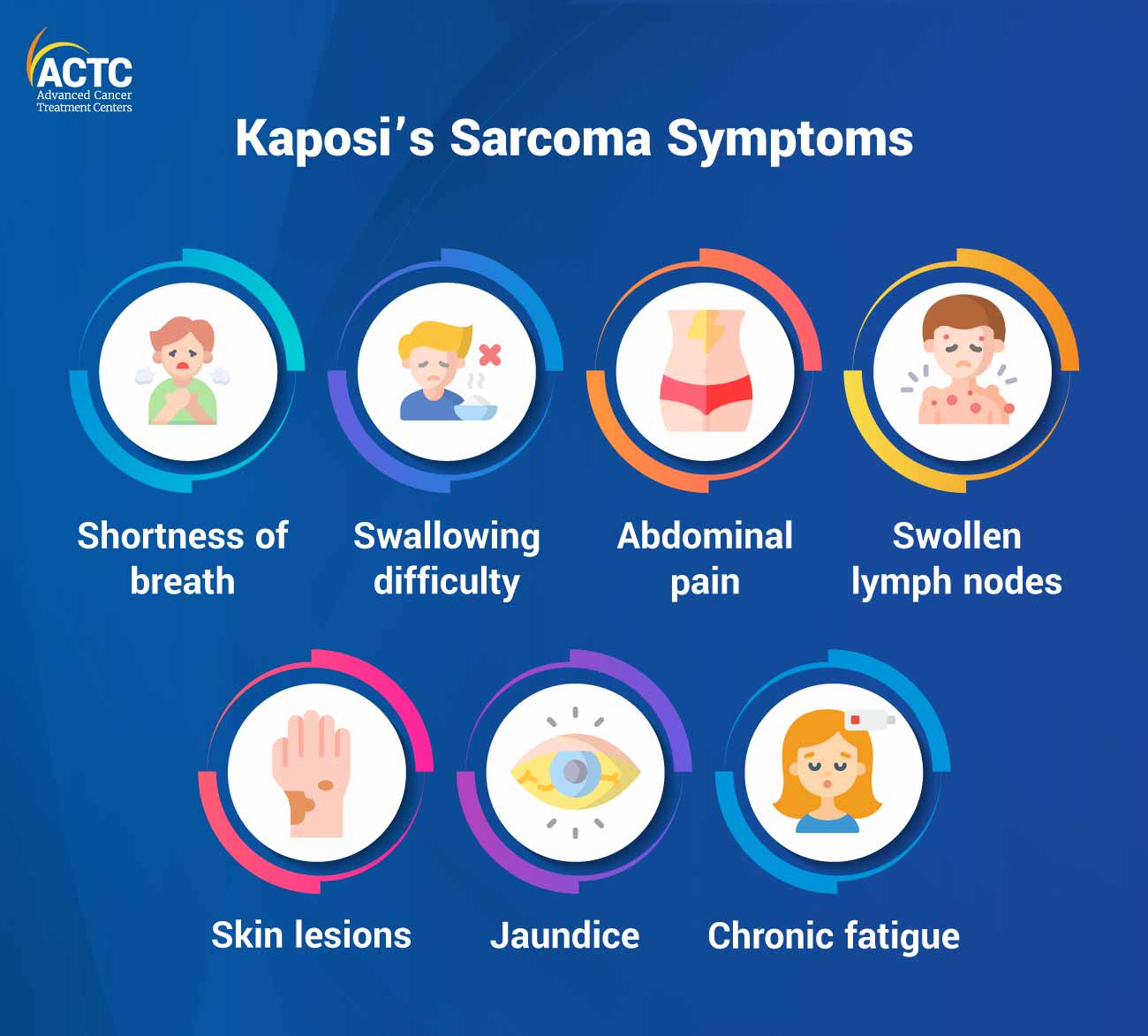
The most common and visible sign of Kaposi's Sarcoma is the development of red, purple, brown or dark skin lesions. These lesions can be flat or have raised nodules or plaques, depending on the type of Kaposi's Sarcoma.
In the early stages, the lesions are often painless and may not cause any discomfort. As the disease progresses, the lesions may become painful, itchy, or tender, especially if they involve mucous membranes or areas of friction.
Read more: 5 Tips for Protecting Your Skin
Kaposi's Sarcoma can affect mucous membranes, leading to lesions in the mouth, nose, throat, or genital areas. These lesions can cause difficulty swallowing, breathing, or bleeding.
In some cases, Kaposi's sarcoma may spread to internal organs, causing shortness of breath, abdominal pain, or jaundice.
The disease may cause enlargement of lymph nodes, particularly in the affected areas.
Kaposi's sarcoma, especially the epidemic associated with HIV, can lead to chronic fatigue and weakness.
Read more: A Complete Guide to Exercise During Cancer Treatment
Individuals with advanced Kaposi's sarcoma may experience the following symptoms:
Fever
Night sweats
Unexplained weight loss
These signs and symptoms are not exclusive to Kaposi's sarcoma and may indicate the presence of other medical conditions. Individuals experiencing any of these symptoms should seek prompt medical attention to receive an accurate diagnosis and appropriate treatment.
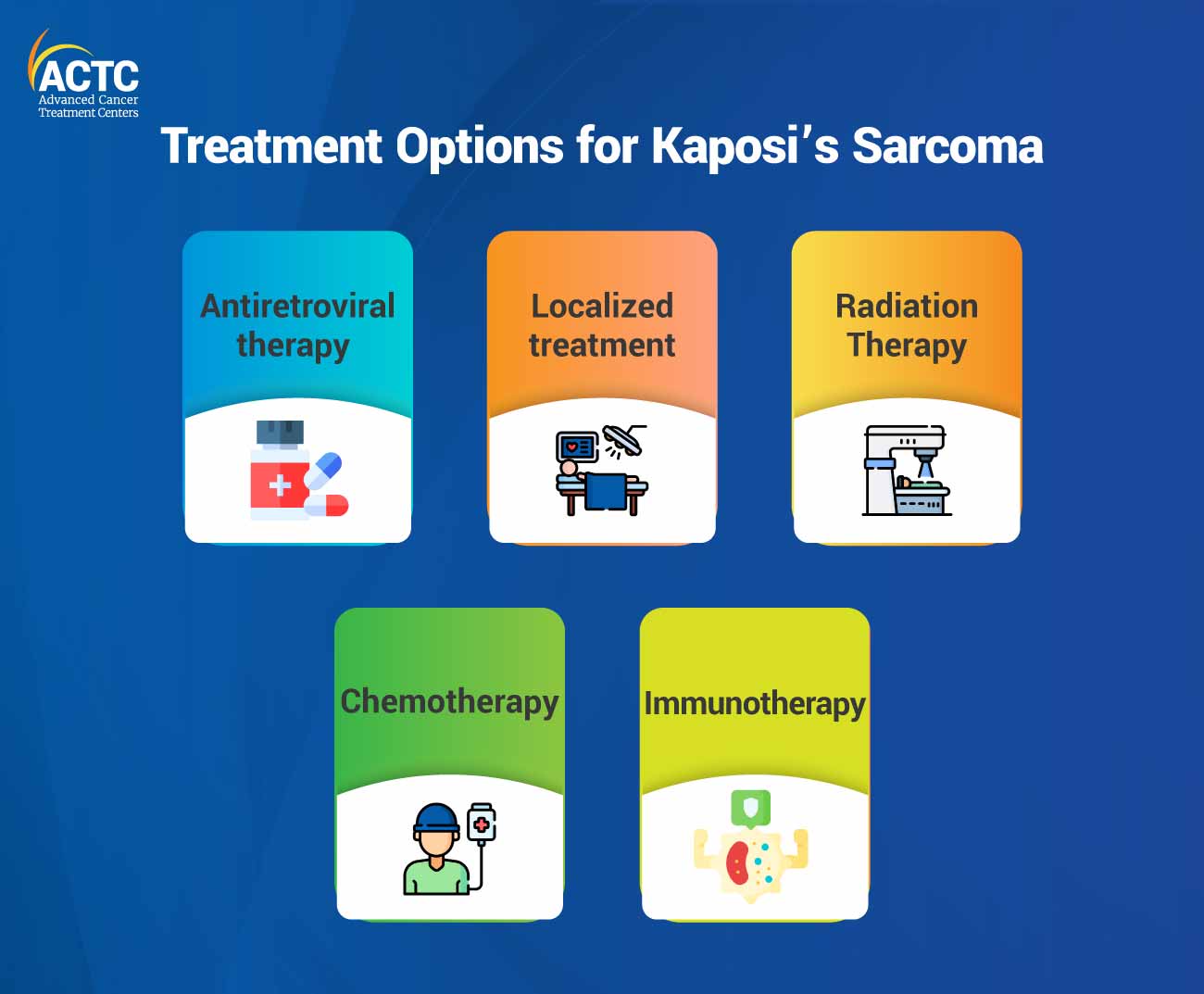
In cases of epidemic Kaposi's Sarcoma, where the disease is associated with HIV infection, antiretroviral therapy (ART) is a fundamental component of treatment. ART helps to suppress the replication of the human immunodeficiency virus (HIV) and boosts the immune system's ability to control Human Herpesvirus 8 (HHV-8). By effectively managing HIV, antiretroviral therapy can slow down the progression of Kaposi's sarcoma and even lead to partial or complete regression of the lesions.
For individuals with localized Kaposi's Sarcoma lesions, oncologists consider a number of treatment options to target specific lesions, which are as follows:
Topical treatment: It involves directly applying prescribed medication to the lesion.
Intralesional therapy: Direct injection of medications, such as chemotherapy agents or immunomodulatory drugs, into the lesions.
Cryotherapy: Freezing the lesions using liquid nitrogen to destroy affected tissues.
Laser therapy: Using focused laser beams to target and destroy Kaposi's Sarcoma lesions.
Excisional surgery: Surgically removing individual lesions in specific cases.
Photodynamic therapy (PDT): It involves applying a unique liquid drug to the skin, which accumulates in tumor cells over a period of hours or days, rendering them sensitive to specific types of light. Once the drug has been absorbed, a specialized light source is directed at the tumor(s), eventually destroying the targeted cells.
Oncologists recommend these types of treatments when Kaposi's sarcoma has spread extensively. Chemotherapy and immunotherapy are the most common systemic treatment options for Kaposi’s sarcoma.
For Kaposi sarcoma (KS) lesions, oncologists typically recommend external beam radiation therapy. In most cases, radiation therapy can effectively treat KS lesions located on or near the body's surface. For visible skin lesions, electron-beam radiation therapy (EBRT) is frequently utilized as it limits side effects and reaches shallow depths.
Typically, radiation treatments for KS lesions are administered once a week for several weeks.
While it may not be possible to completely prevent Kaposi's sarcoma, certain measures can help reduce its risk. Individuals living with HIV should consult their healthcare providers to strengthen their immune system. Additionally, individuals should practice safe sex and get regular STI screenings. Adequate sun protection can also reduce the risk of this cancer.
Prior to the AIDS epidemic, Kaposi sarcoma (KS) was rarely diagnosed in the United States, with approximately 2 new cases found annually for every million people. However, with the onset of the AIDS epidemic, the incidence of KS in the country skyrocketed. In the early 1990s, the rate of KS peaked at around 47 cases per million people per year. Therefore, individuals should consider preventive measures and seek immediate medical attention if they experience any symptoms. Early detection and prompt medical intervention can increase the chances of a better outcome from the treatment.
For any queries or concerns about Kaposi’s sarcoma, contact the Advanced Cancer Treatment Center. We are one of the best cancer centers in Florida, specializing in personalized cancer treatment.


January 07, 2026
A chemo port is a small device placed under your skin that makes recei...
KNOW MORE
December 24, 2025
It's natural to wonder if testosterone replacement therapy (TRT) is sa...
KNOW MORE
December 24, 2025
A rash that will not calm down is scary, especially when it changes or...
KNOW MORE
December 24, 2025
Florida’s lung cancer burden remains significant and affects many fa...
KNOW MORE
December 24, 2025
A partial hysterectomy, also called a supracervical hysterectomy, is s...
KNOW MORE
December 24, 2025
Finding a rash on your breast can be unsettling, but remember, many ra...
KNOW MORE
