
Book a Consultation
Thank you!
Your form has been sent successfully.

An Islet cell tumor originates in the neuroendocrine cells of the pancreas. It is also called a pancreatic neuroendocrine tumor (pNETs). Neuroendocrine cells form clusters of cells called islets of Langerhans, which produce hormones like insulin and glucagon. They re responsible for regulating the blood sugar level.
Islet cell tumors may be benign (non-cancerous) or malignant (cancerous). Malignant pancreatic NETs are known as pancreatic endocrine cancers or islet cell cancer.
Based on hormones produced, islet cell tumors can be divided into functional or non-functional tumors.
This kind of tumor produces excessive hormones. The tumor can be further classified according to the origin of the cells.
| Name of Functional Islet Cell Tumor | Cells that form the tumor |
|---|---|
| Insulinoma | Insulin-making cells |
| Glucagonomas | Cells that make glucagon |
| Gastrinoma | Cells that secrete gastrin |
| Somatostatinoma | Somatostatin-releasing cells |
| VIPomas | Vasoactive intestinal peptide-producing cells |
| ACTH-secreting tumors | Cells that produce adrenocorticotropic hormone (ACTH) |
These tumors don't release excess hormones and cause fewer symptoms than functional islet cell tumors. Due to this, they are often diagnosed at a later stage when their size increases considerably.
These tumors may show symptoms either because of their growth or the excessive production of hormones. Non-functional Islet cell cancer may grow and spread to other body parts before causing signs and symptoms.
Non-functional islet cell tumor symptoms may include:
 Diarrhea
Diarrhea
 Indigestion
Indigestion
 Lump in the abdomen
Lump in the abdomen
 Pain in the back or abdominal area
Pain in the back or abdominal area
 Generalized yellowing of the skin (jaundice)
Generalized yellowing of the skin (jaundice)
Functional islet cell tumor symptoms depend on the excessive hormones secreted by the tumor.
| Functional Islet Cell Tumor | Symptoms of Functional Islet Cell Tumor |
|---|---|
| Gastrinoma | Stomach ulcers, abdominal pain, gastroesophageal reflux |
| Insulinoma | Fast heart rate, low blood sugar, blurry vision, lightheadedness, confusion |
| Glucagonoma | Skin rash, high blood sugar, blood clots, weight loss, sore tongue |
| VIPomas | Watery diarrhea, dehydration, abdominal cramps, weight loss, weakness |
| Somatostatinoma | High blood sugar, foul-smelling stool that floats (steatorrhea), diarrhea, weight loss, yellowness of skin |
Treatment options for islet cell cancer depend on the type, stage, and overall health of the patient.
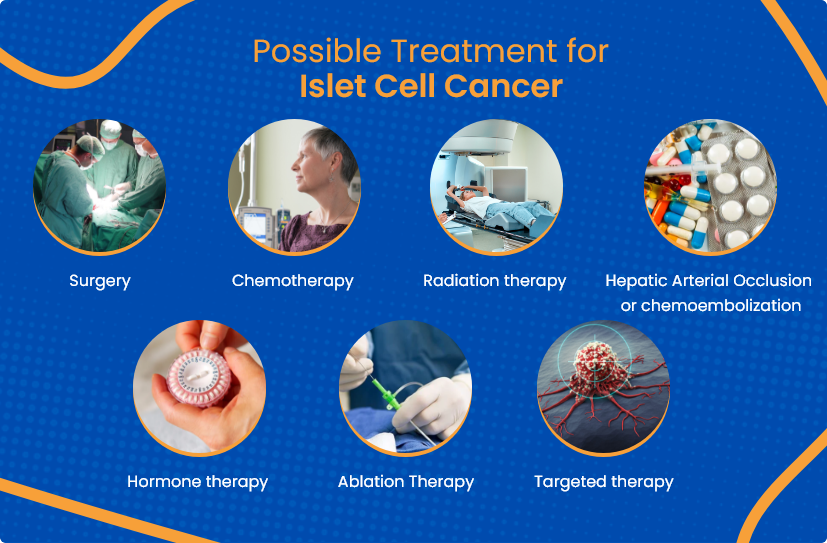
Oncologists surgically remove the tumor with some surrounding healthy tissue. They may perform a minimally invasive surgical technique called laparoscopic surgery, depending on the location and size of the tumor. Surgical removal is the preferred treatment for islet cell cancer.
Chemotherapy uses anti-cancer drugs injected intravenously or orally, which enter the bloodstream and reach and destroy rapidly growing cancer.
Radiation therapy uses high-energy radiation to kill cancerous cells to treat islet cell cancer. Radiation can be delivered via an external machine outside the body, called external beam radiotherapy.
Anti-cancer drugs are administered through a catheter into the hepatic artery. The drug is mixed with a specific agent that blocks the blood flow to the tumor, thereby destroying cancerous cells.
This therapy balances hormone levels in the body by blocking the effects of excessive hormones produced by the functional islet cell tumor.
Ablative treatments are usually used when the tumor spreads to other body parts. It reduces the size and improves symptoms of this cancer. It uses extreme heat, cold, or high-energy radio waves to destroy tumor cells.
Targeted drug therapy explicitly targets specific cell proteins or genes that block the growth and spread of cancer. It causes fewer side effects and spares healthy cells because of its specific action.
The following tests and procedures may be recommended depending on the symptoms, age, and general health:
Blood and urine samples are tested to check the abnormal level of hormones, glucose, and other substances (chromogranin A and c-peptide).

A biopsy is a definitive cancer diagnosis that includes removing a tissue sample for microscopic examination. A biopsy can be performed using a fine needle to remove tissue fluid or cells from the suspicious area (FNAC) or surgically remove a part or entire tumor.

A biomarker test is a molecular test that identifies specific genes, proteins, and other factors that are unique to this type of tumor.
High-intensity radiation is used to produce detailed 3-dimensional computerized images. They are used to locate and measure the tumor's size. Various imaging tests used are:
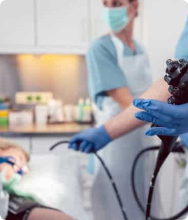
Endoscopic ultrasound or endo-sonography uses a probe attached to a thin, flexible, lighted tube called an endoscope. It is inserted into the body through the mouth or rectum. The probe uses high-energy sound waves. The organs reflect the sound waves, creating an image of the pancreas and other body organs.
The oncologists at ACTC, Florida, are dedicated to providing exceptional patient care - prescribing effective personalized and evidence-based treatment plans for their patients. We strive to establish a positive environment for patients and their families throughout their cancer journey, simultaneously focusing on physical and mental health. We have some of the most accomplished cancer specialists working on our team.
The following are our providers who you can consult at ACTC:

MD, Hematology & Oncology

MD, Ph.D., Hematology/ Medical Oncology

MD, Radiation Oncologist

If you or a loved one has been diagnosed with islet cell cancer, a detailed discussion with your primary physician will help you understand your condition better. Your PCP can then refer you to an advanced specialty center such as ACTC in Florida.
As one of Florida's best cancer centers, we understand how a cancer diagnosis and therapy impact a person's physical and emotional well-being. Therefore, we work hard to make patients and their families feel secure. We understand how imperative it is for you and your loved one to make informed choices and play an active part in your medical care. We at ACTC strive to support you at every step of diagnosis, staging, treatment, and long-term follow-up in one convenient location. Our cancer specialists are supported by qualified clinical staff with over two decades of experience and a reputation for providing personalized cancer treatment.
Schedule a consultation by calling
 352-345-4565
352-345-4565
According to the American Cancer Society, islet cell cancer comprises less than 2% of pancreatic islet cell tumors.
Various factors that determine the prognosis are- the patient's general health and age, location of the tumor, metastasis of the tumor, if the patient has MEN1 syndrome, or if cancer has recurred.
Islet cell tumors are usually slow-growing tumors. They may be cured with pancreatic resection surgery if localized to the pancreas and regional lymph nodes.
Schedule a consultation by calling
 352-345-4565
352-345-4565