
Book a Consultation
Thank you!
Your form has been sent successfully.

Learning that melanoma is a form of skin cancer can feel overwhelming, but understanding it is an important first step. Melanoma begins in melanocytes—the cells that make melanin, the pigment responsible for your skin and hair color. Melanin also plays a role in shielding your skin from harmful UV rays.
While melanoma isn’t the most common skin cancer, it’s known for spreading more quickly than other types, which is why early detection is so critical. It can appear anywhere on your body, but it most often shows up on the chest or back in men, and the legs in women.
There are several types of melanoma, each named for how or where they grow. Some spread slowly on the skin's surface, while others move deeper quickly.
Superficial spreading melanoma: This is the most common type, making up about 70% of cases. It often grows across the skin for years before moving deeper.
Nodular melanoma: About 15% of melanomas are nodular. They quickly grow deeper into the skin, making early detection important.
Acral-lentiginous melanoma: This type typically appears on palms, soles, or under nails, especially in people with darker skin. While this melanoma can appear subtle at first, it's often diagnosed later, which is why regular skin checks are important.
Lentigo maligna melanoma: Usually appearing on sun-exposed skin such as the face or neck, this type can slowly grow for many years before becoming invasive.
Amelanotic melanoma: Rare and hard to spot because it lacks color, this melanoma often changes shape or size and has irregular borders.
Desmoplastic melanoma: This uncommon type is often aggressive locally and typically appears on the head or neck of older adults. It may look like scar tissue.
A new or changing spot on your skin may be a sign of melanoma. Check your skin regularly using the ABCDE rule:
Asymmetry: One half of the mole doesn't match the other.
Border: The edges are uneven, blurred, or hard to define.
Color: The spot may be dark brown, black, or contain unusual colors like white, gray, red, or blue.
Diameter: Melanomas usually grow larger than the size of a pencil eraser (6 mm).
Evolving: The spot changes size, shape, or color over time.
Not all melanomas are dark or obvious. Any mole or spot that seems to be growing or changing should be evaluated by a doctor promptly.
A biopsy is the only way to confirm melanoma. During a biopsy, your doctor removes a small tissue sample from the suspicious spot to check under a microscope.
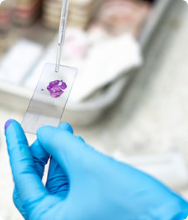
Your doctor will numb the area first, so while you may feel a quick pinch or pressure, most people find the biopsy quite tolerable. Biopsies can be incisional (removing just part of the spot) or excisional (removing the whole spot).
If melanoma is found, your doctor may recommend imaging tests to see if it has spread:
CT scans: Create detailed pictures of your organs.
MRI: Used especially for checking the brain and spinal cord.
PET-CT scan: Shows detailed images of the whole body and can identify areas where melanoma might have spread.
Your melanoma treatment plan depends on the type and stage of your cancer, as well as your overall health.
Your doctor will discuss the best approach for your situation, which might include surgery, radiation therapy, chemotherapy, targeted therapy, or immunotherapy.
Surgery is the main treatment for melanoma. To treat the cancer, your doctor will take out the melanoma with some healthy skin and may also remove nearby lymph nodes if needed.
Radiation therapy uses powerful energy beams to kill cancer cells. It's sometimes used after surgery to target any remaining cancer cells or in places where surgery is difficult.
Chemotherapy uses special drugs given through an IV or by mouth to reach and kill cancer cells throughout your body. It targets rapidly dividing cells, which include melanoma cells.
Targeted therapy drugs work by blocking specific proteins or genes that help melanoma grow and spread. Because they focus on specific cancer targets, they tend to cause fewer side effects compared to traditional chemotherapy.
Also known as biologic therapy, immunotherapy helps your body's immune system attack cancer cells. It uses special proteins to boost your own immune response against melanoma.
The team at ACTC in Florida is dedicated to compassionate, individualized cancer care that reflects each patient’s unique needs and medical history.
We strive to create a healing environment that nurtures both the body and mind at every stage of your journey.
Meet the experts who are here to guide you at ACTC:

Hematology/Oncology

Hematology/Oncology

Radiation Oncology
At ACTC in Florida, you’re supported by a team of expert cancer specialists and clinical staff with over 20 years of experience. We’re with you every step—from diagnosis to long-term follow-up—all under one roof.
Call 352-345-4565 or book an appointment.

If you or a loved one has been diagnosed with melanoma, a detailed discussion with your primary physician will help you understand your condition better. Your primary care doctor can then refer you to an advanced specialty center, such as ACTC in Florida.
As one of Florida's best cancer centers, we understand how a cancer diagnosis and therapy impact a person's physical and emotional well-being. Therefore, we work hard to make patients and their families feel secure. We understand how imperative it is for you and your loved one to make informed choices and play an active part in your medical care. We at ACTC strive to support you at every step of diagnosis, staging, treatment, and long-term follow-up in one convenient location. Our cancer specialists are backed up by qualified clinical staff with over two decades of experience and a reputation for providing personalized melanoma treatment.
Schedule a consultation by calling
 352-345-4565
352-345-4565
Melanoma is the fifth most common cancer in the U.S. among both men and women, according to the American Society of Clinical Oncology. Although it can occur at any age, melanoma is more frequently diagnosed in older adults, particularly those over age 50.
The main risk factors for melanoma include excessive sun exposure (particularly sunburns), fair skin, a personal or family history of skin cancer, having many moles or atypical moles, and a weakened immune system.
You can help reduce your risk by limiting sun exposure, wearing protective clothing and sunglasses, regularly using sunscreen with an SPF of 30 or higher, and avoiding tanning beds.
Studies suggest that about 8% of melanoma patients may develop another type of cancer. If you’ve had melanoma, your biggest risk is developing another skin cancer, which is why ongoing checkups matter.
Yes, melanoma can spread (metastasize) to other areas of the body. Common areas where melanoma spreads include lymph nodes, lungs, liver, brain, bones, and occasionally the stomach or intestines.
Your chances of recovery from melanoma depend on several factors, such as tumor thickness, type, stage, location on your body, and your age and overall health. Melanomas less than 1 mm thick typically have a more favorable outlook. Melanomas located on the arms and legs generally have a better prognosis compared to those on the trunk, head, or neck. Discuss your personal prognosis with your doctor.
Schedule a consultation by calling
 352-345-4565
352-345-4565