
Book a Consultation
Thank you!
Your form has been sent successfully.


February 07, 2023
Immunotherapy has revolutionized cancer treatment in recent years, offering hope to many patients who may not have responded to other forms of treatment. It is an emerging form of cancer treatment that utilizes the body's own immune system to fight rapidly growing, abnormal cells. The immune system is the body's natural defense system that helps protect against infections, diseases, and other harmful substances. It is made up of a network of cells, tissues, and organs that work together to identify and destroy substances that are foreign or harmful to the body.
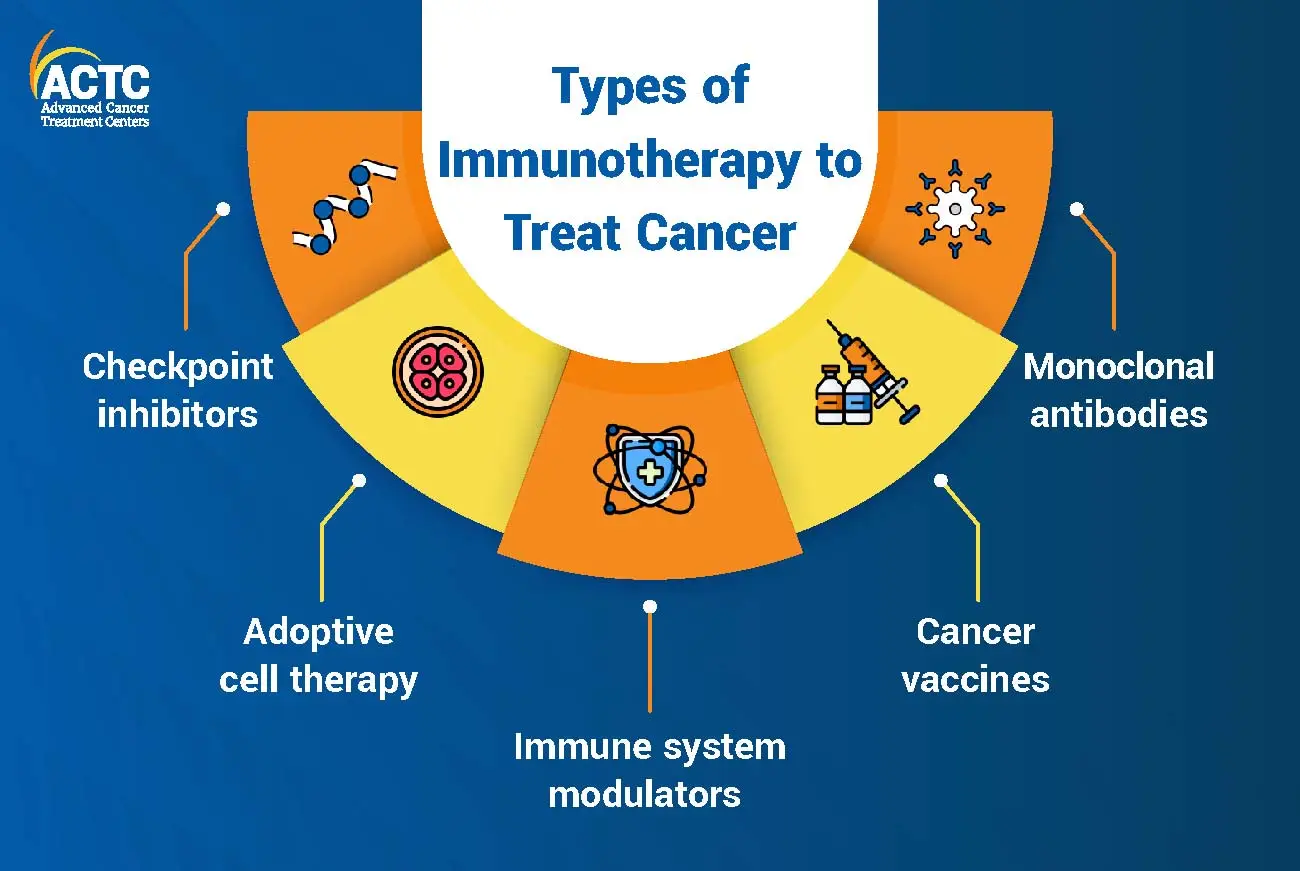
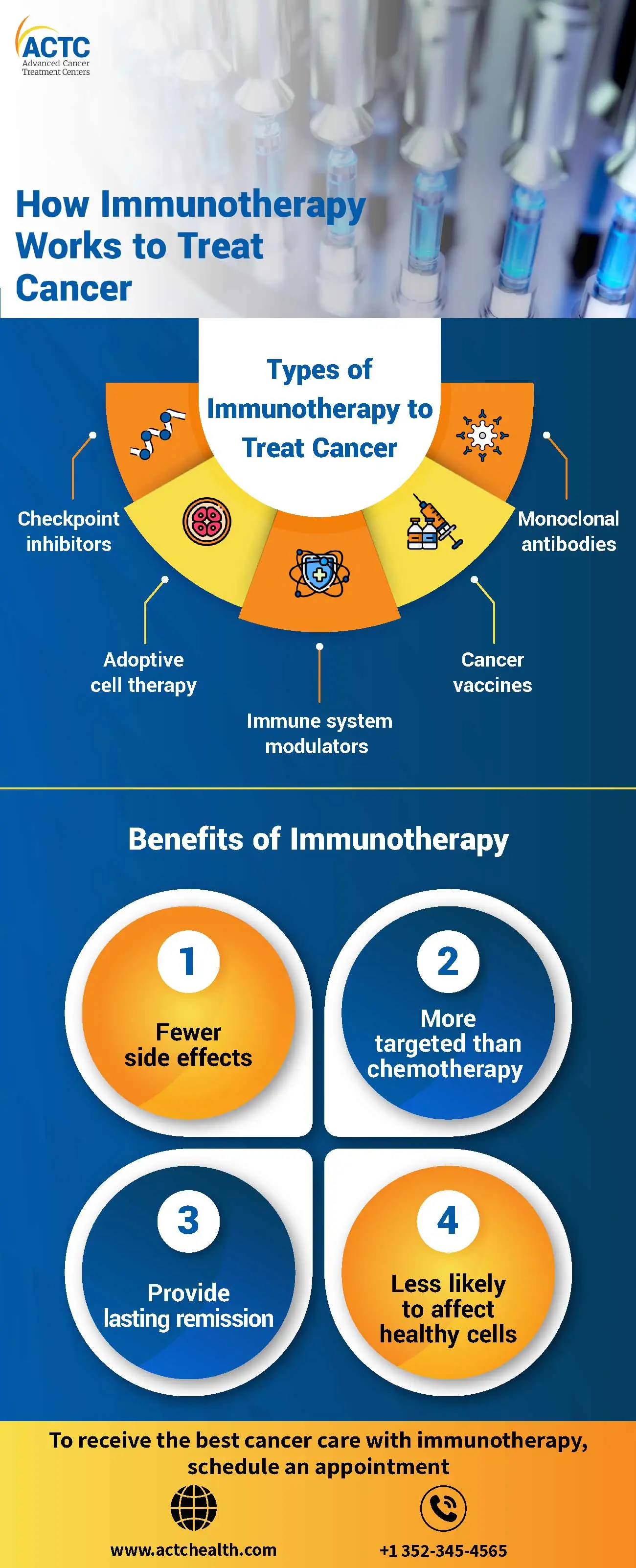
The scope of immunotherapy for cancer is a promising area of research and is being explored as a potential treatment option for a variety of types of cancer. There are several different types of immunotherapies, each of which works in a slightly different way to stimulate the immune system to attack cancer cells.
Read More: Making the Best of Life After Cancer
It is a type of immunotherapy that works by blocking specific proteins that inhibit the immune system's ability to recognize and attack abnormal cells. These proteins, called immune checkpoints, help regulate the immune system and prevent it from attacking normal, healthy cells. By blocking these checkpoints, checkpoint inhibitors can help the immune system recognize and attack cancer cells more effectively.
Checkpoint inhibitors are often used to treat melanoma, lung cancer, and kidney cancer.
Also known as T-cell transfer therapy, this is a type of immunotherapy for cancer that involves the transfer of immune cells called T-cells from the patient's own body to the affected site. These T-cells are trained to recognize and attack cancer cells and can be very effective at destroying them.
Adoptive cell therapy is typically used to treat melanoma.
This immunotherapy involves the use of man-made proteins that are designed to bind to specific proteins in cancer cells. These proteins, called antigens, are found on the surface of the abnormal cells and help the immune system recognize and attack the cells. By binding to these antigens, monoclonal antibodies can help the immune system recognize and attack cancer cells more effectively.
Monoclonal antibody therapy is often used to treat breast and colon cancer.
These are designed to stimulate the immune system to recognize and attack cancer cells. They can be used to prevent or treat cancer that has already developed. There are several different types of vaccines, including preventive vaccines and therapeutic vaccines. Preventive vaccines are given to people who are at high risk of developing cancer, while therapeutic vaccines are given to people who have already been diagnosed with cancer.
Cancer vaccines are often used to treat prostate cancer and breast cancer.
This is a type of immunotherapy that works by altering the way the immune system functions. They can be used to stimulate the immune system to attack cancer cells more effectively, or to suppress the immune system to prevent it from attacking normal, healthy cells.
Immune system modulators are often used to treat autoimmune diseases, such as rheumatoid arthritis and multiple sclerosis, as well as cancer.
Read More: A Complete Guide to Exercise During Cancer Treatment

One of the primary benefits of immunotherapy is that it generally has fewer side effects than other types of cancer treatment, such as chemotherapy. This is because immunotherapy is more targeted and specifically targets the affected cells, rather than attacking all rapidly dividing cells in the body. As a result, patients who receive immunotherapy may not experience severe side effects of cancer treatment including nausea, vomiting, and hair loss.
Unlike chemotherapy, which attacks all rapidly dividing cells in the body, immunotherapy is more targeted and specifically targets cancer cells. Therefore, it works more efficiently to destroy cancer cells and can lead to fewer side effects along with a better quality of life for patients.
Some patients who receive immunotherapy may achieve lasting remission, meaning that their cancer goes into complete remission and does not return. This is especially true for patients with certain types of cancer, such as melanoma and lung cancer, who may have a better chance of achieving long-term remission with immunotherapy.
Because immunotherapy is more targeted and specifically targets abnormal cells, it is less likely to affect healthy cells and tissues. Therefore, the risk of additional damage to the healthier cells is minimized and there are better chances of quick recovery.
Like any medical treatment, immunotherapy for cancer can have potential risks and side effects. Some common side effects of immunotherapy include:
Inflammation: Immunotherapy can sometimes cause inflammation in different parts of the body, such as the lungs, liver, and intestines. This can lead to symptoms such as shortness of breath, abdominal pain, and diarrhea.
Autoimmune reactions: Immunotherapy works by activating the immune system and for that reason, it can sometimes lead to autoimmune reactions, in which the immune system mistakenly attacks healthy cells and tissues in the body. This can cause symptoms such as rash, joint pain, and kidney damage.
Toxicity: Some types of immunotherapies can be toxic to certain organs, such as the liver or kidneys, and may lead to organ damage.
Other side effects: Other potential side effects of immunotherapy include fatigue, fever, nausea, vomiting, and loss of appetite.
It is important to discuss the potential risks and side effects of immunotherapy with your doctor before starting treatment. Your doctor can help you weigh the potential benefits and risks of immunotherapy and determine if it is the right treatment option for you.
Immunotherapy can be an effective treatment option when used in combination with other treatments, such as chemotherapy, radiation, or surgery. It is important to discuss all treatment options with the healthcare provider in order to determine the best course of treatment. Consult a primary care physician or a healthcare provider to help weigh the potential benefits and risks of each treatment option and determine the best course of action.
Looking for the best cancer care? Contact ACTC, one of the best cancer treatment centers in Brooksville and schedule an appointment with our board-certified oncologists.


January 07, 2026
A chemo port is a small device placed under your skin that makes recei...
KNOW MORE
December 24, 2025
It's natural to wonder if testosterone replacement therapy (TRT) is sa...
KNOW MORE
December 24, 2025
A rash that will not calm down is scary, especially when it changes or...
KNOW MORE
December 24, 2025
Florida’s lung cancer burden remains significant and affects many fa...
KNOW MORE
December 24, 2025
A partial hysterectomy, also called a supracervical hysterectomy, is s...
KNOW MORE
December 24, 2025
Finding a rash on your breast can be unsettling, but remember, many ra...
KNOW MORE
