
Book a Consultation
Thank you!
Your form has been sent successfully.



July 06, 2023
The thyroid gland is located in the neck and produces hormones to regulate the body’s metabolic rate. Although thyroid cancer is relatively rare, it can pose serious health risks if not detected and treated in time.
When it comes to thyroid cancer treatment, determining the right approach depends on several factors. However, the most crucial factor is the stage of the cancer. Healthcare providers determine the stage after examining the extent and severity of the disease.
In this blog post, we will share detailed information about the diagnostic procedures for this cancer, its stages, and treatment options. Read on to learn more.
The following are the most common types of thyroid cancer:
It is the most common type, accounting for approximately 80% of all thyroid cancer cases. This type of thyroid cancer usually grows slowly and is mostly curable when diagnosed early.
It is less common than papillary, accounting for 10-15% of all cases. It is also a slow-growing cancer, often curable if diagnosed and treated early.
This type is much less common and accounts for only 4% of cases. Medullary thyroid cancer can be more aggressive than papillary or follicular cancers and may require more aggressive treatment.
This is the rarest yet most aggressive type, accounting for less than 2% of all thyroid cancer cases. Anaplastic cancer spreads rapidly and is often difficult to treat.
To diagnose this disease, physicians may use a number of different medical tests to check the presence of cancer and determine its spread.
First, primary care physicians perform a physical examination to check for any unusual growth or swelling in the neck, thyroid gland, throat, or lymph nodes.
Blood tests are done to help check thyroid hormone levels and thyroid-stimulating hormone levels. It also helps identify tumor markers like thyroglobulin (Tg) and thyroglobulin antibodies (TgAb). The tumor marker test is done mostly when the physician suspects medullary thyroid cancer (MTC).
Healthcare providers recommend an ultrasound, an X-ray, or a CT scan to get a clearer picture of the internal organs, including the size of the thyroid gland and any nodules. It can help identify whether a nodule is solid or a cyst.
A biopsy is the only way to confirm cancer diagnosis because it helps determine whether a nodule is cancerous or benign. It can be done in two ways: fine needle aspiration or surgical biopsy. During the needle aspiration biopsy, if the results are not definite, the physician may suggest surgery to remove the nodule as well as the affected lobe of the thyroid.
Radionuclide scanning can be done to learn more about the thyroid nodule and determine the stage. This process involves the use of a small amount of radioactive iodine.
Once the diagnosis is confirmed, oncologists proceed with staging to determine the best course of treatment for this disease.
Oncologists use the TNM classification system to determine the stage of thyroid cancer. T stands for the size of the primary tumor and explains whether it has spread to nearby tissues or structures. While N indicates whether the cancer has spread to nearby lymph nodes, M suggests whether the cancer has metastasized and spread to distant organs in the body.
The following are thyroid cancer stages based on the TNM classifications:
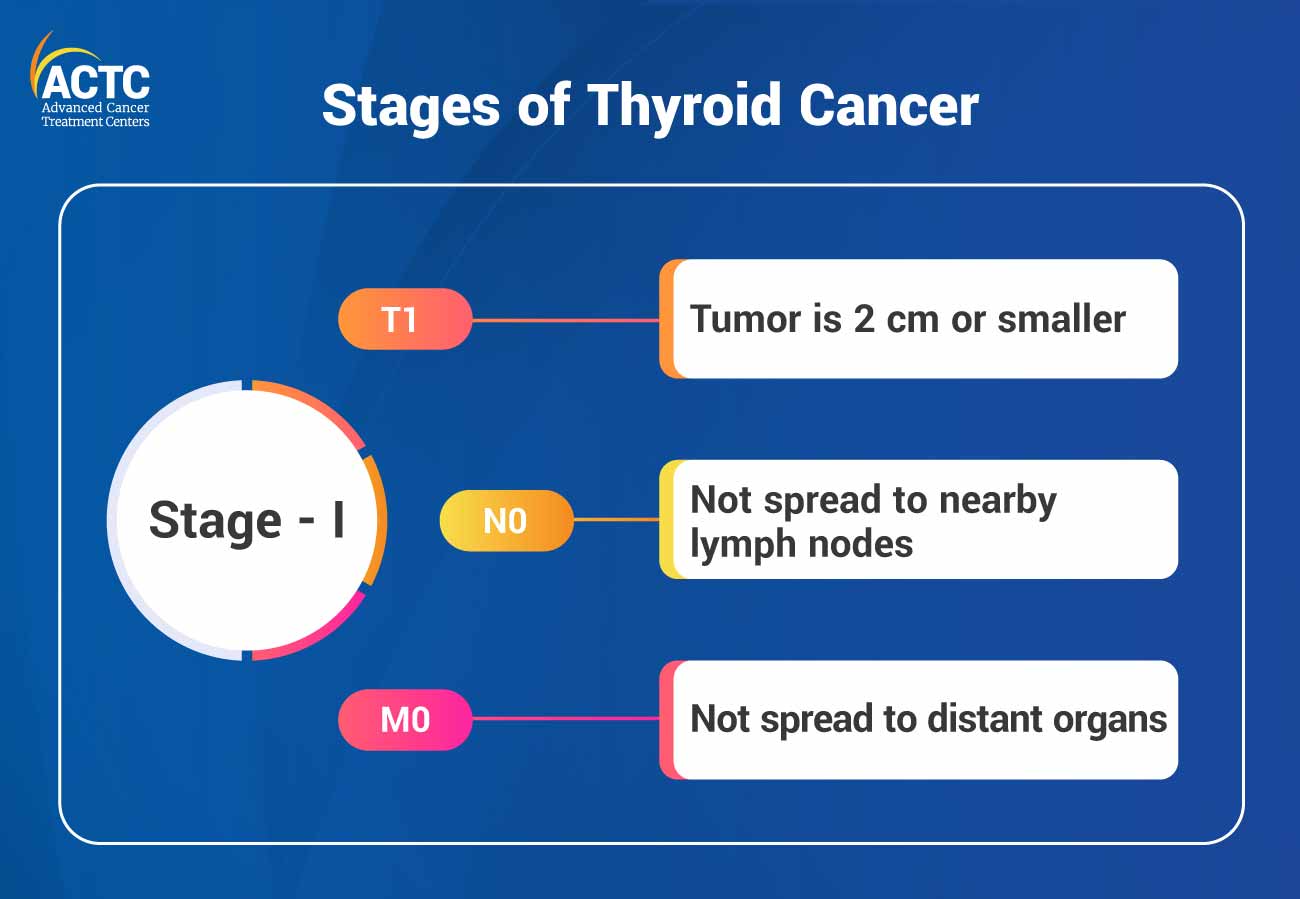
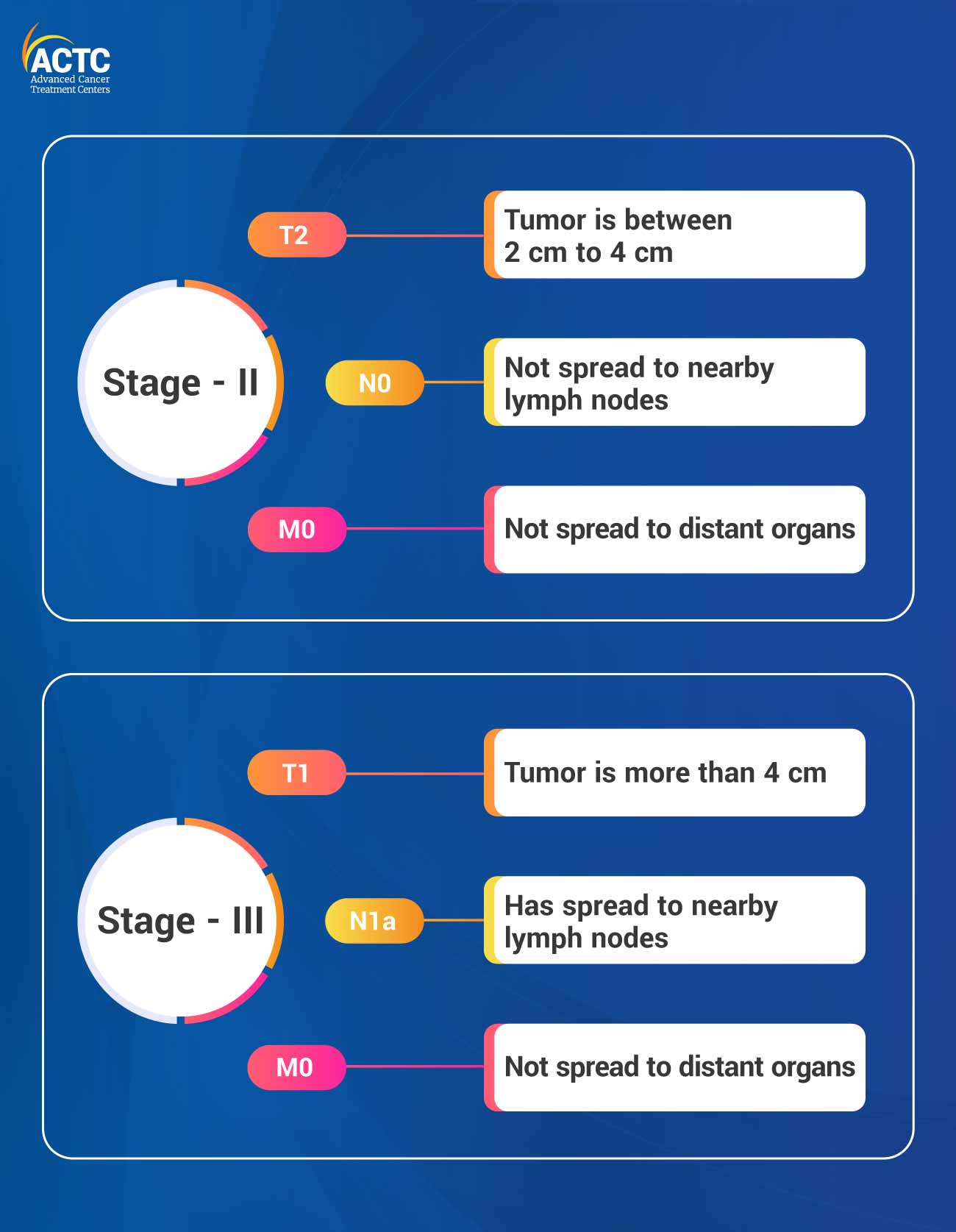


It is the most common treatment option for thyroid cancer. Oncologists determine the type of surgery depending on the size, location, and stage of the cancer. There are mainly three types of thyroid surgery which are as follows:
Thyroidectomy: It is the most common type of surgery that involves the removal of the thyroid gland. Surgeons may opt for a total or a partial thyroidectomy, depending on the spread of the disease.
Lobectomy: This surgical procedure involves the removal of one lobe of the thyroid gland and is typically used for small, localized tumors.
Lymph node dissection: In this procedure, surgeons remove the affected lymph nodes in the neck to prevent the spread of cancer.
Surgery is generally performed under general anesthesia, and the recovery period can vary depending on the type of surgery performed.
Oncologists recommend radioactive iodine primarily for individuals who have had their entire thyroid gland removed. It is typically the case for intermediate or high-risk papillary or follicular cancer. RAI is a form of targeted radiation therapy that involves the use of radioactive iodine to destroy any remaining cancerous cells after surgery.
This thyroid cancer treatment procedure may produce side effects such as nausea, dry mouth, or a metallic taste in the mouth. However, these symptoms are usually temporary and go away within a few days.
Once the entire thyroid gland is removed, the body can’t produce the thyroid hormones required to regulate metabolism. This treatment option uses synthetic thyroid hormones to replace the hormones that the thyroid gland would normally produce. Hormone therapy is also usually used after thyroidectomy, which is mainly done for papillary or follicular cancer.
Additionally, hormone therapy helps maintain thyroid hormone levels in the body and reduces the risk of recurrence. Oncologists may also suggest regular blood tests to monitor TSH levels and adjust the dosage accordingly.
Oncologists often recommend radiation therapy after surgery to kill any remaining cancerous cells which they couldn’t remove during surgery. They may also use it to shrink a tumor before surgery or to relieve symptoms such as swallowing issues.
In the case of thyroid cancer, radiation oncologists usually recommend external beam radiotherapy where they use a machine to deliver high-energy radiation to the affected area. It is typically used for individuals suffering from anaplastic or medullary thyroid cancer, or whose cancer has metastasized extensively.
This traditional treatment procedure is not a commonly used treatment option for thyroid cancer because the cancerous cells are generally not very responsive to it. Oncologists prescribe chemotherapy for individuals suffering from advanced or aggressive forms of thyroid cancer. They recommend it in combination with other thyroid cancer treatments for those suffering from anaplastic or medullary thyroid cancer, or whose cancer has metastasized and spread to other parts of the body.
Chemotherapy drugs can cause several mild or severe side effects, including nausea, hair loss, fatigue, and increase the risk of infection as well.
Read more: 6 Essential Dos and Don'ts for Post-Chemotherapy Recovery
It involves the use of drugs to target specific molecules that helps in the growth and spread of cancerous cells. Healthcare providers typically use it for individuals with advanced or recurrent thyroid cancer who have not responded to other treatments.
Tyrosine kinase inhibitors (TKIs) are the most used targeted therapy that help block the activity of certain enzymes that promote the growth and spread of cancer cells.
Thyroid cancer can be a challenging diagnosis to face, but with proper treatment and follow-up care, it is possible to lead a healthy and fulfilling life. Individuals should not miss or delay any follow-up check-ups to ensure that the cancer has not recurred. It will also help the healthcare team to monitor any potential long-term side effects of treatment. Seek support from loved ones, join support groups, stay engaged in self-care activities, and consult a professional to help manage the emotional impact of thyroid cancer.
For any queries about thyroid cancer and its treatment options, contact Advanced Cancer Treatment Centers, one of the best cancer centers in Florida, providing personalized cancer treatment plans.


June 03, 2024
The last decade has witnessed a sea change in oncologic treatments. Re...
KNOW MORE

April 17, 2024
Oncology is one of the most exciting fields in medicine today. Disease...
KNOW MORE

February 28, 2024
By taking steps to prioritize colon health, we can promote knowledge a...
KNOW MORE

February 21, 2024
Women must prioritize their breast health by engaging in regular breas...
KNOW MORE

February 16, 2024
Understanding the complexities of Salivary Gland Cancer is extremely i...
KNOW MORE

February 14, 2024
With this guide, we hope to empower individuals to take proactive step...
KNOW MORE
