
Book a Consultation
Thank you!
Your form has been sent successfully.


May 01, 2026
If you or someone in your family is facing a colon cancer concern, the language can feel overwhelming. This guide is for patients and caregivers in Brooksville and across Hernando County who want clear answers before the next appointment.
Colon cancer starts when cells in the colon begin to grow in ways they should not. The colon is part of the large intestine, the muscular tube that absorbs water from food and forms stool. The rectum is the final section of the large intestine, connecting the colon to the anus.
Colon cancer specifically starts in the colon. The umbrella term colorectal cancer covers cancers that start in either the colon or rectum. Many begin as small growths called polyps on the inner lining, and some change into cancer over years.
Found early, certain polyps can be removed before they ever turn into cancer. The prevention angle worth knowing is covered in colon polyps all you need to know about them. Early colon cancer often causes no symptoms, so waiting until something feels wrong is not a safe screening plan.
Risk does not equal diagnosis, and most people with risk factors will never develop colon cancer. Knowing your own picture helps you and your primary care doctor decide when to start screening.
Health-history factors that raise risk include:
Age: Risk rises after 45, and most diagnoses occur in adults 50 and older.
Inflammatory bowel disease: Crohn's disease or ulcerative colitis over many years.
Personal or family history: A prior colon cancer or polyp finding, or a close relative who had either.
Inherited syndromes: Lynch syndrome and familial adenomatous polyposis (FAP) raise lifetime risk and often shift screening earlier.
Daily habits also play a part. Risk tends to be higher with low physical activity, a fiber-poor diet, excess body weight, heavy alcohol use, or tobacco use.
The practical playbook in Steps to a healthy colon: preventing polyps is a good starting point with your doctor.
Colon cancer can be quiet for a long time. Many people are diagnosed during routine screening before any warning signs appear. When symptoms do show up, they tend to be persistent rather than one-off.
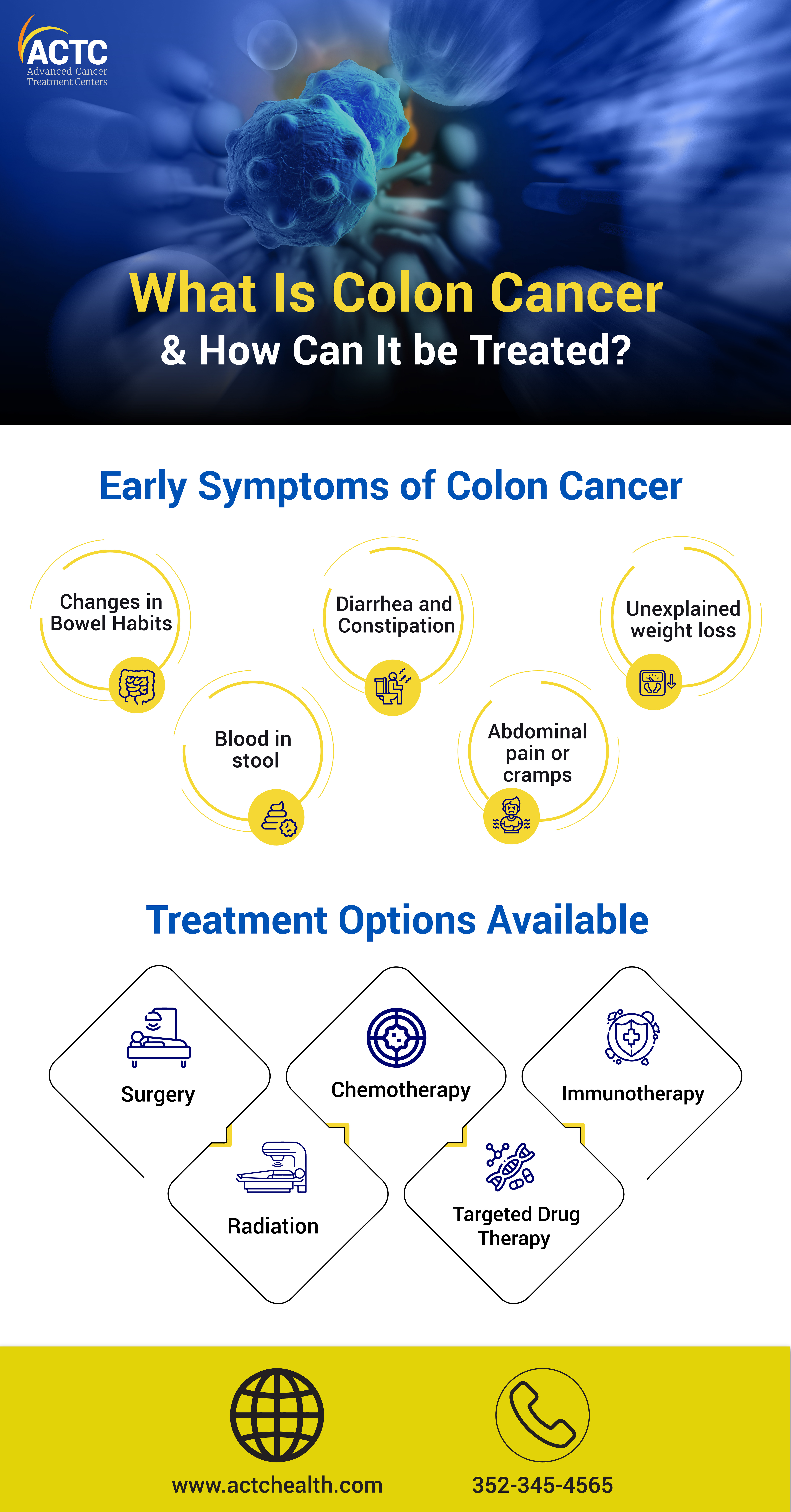
Common symptoms worth bringing to a doctor include:
Blood in or on your stool, or stool that looks dark or tarry
A lasting change in bowel habits: new constipation, diarrhea, or narrower stools
Abdominal pain, cramping, or a feeling of incomplete emptying that does not go away
Unexplained weight loss
Fatigue or weakness, sometimes from low iron levels
A single symptom rarely means cancer. Still, rectal bleeding, dark stool, unexplained weight loss, low iron, or a persistent bowel change is a reason to call your doctor rather than wait. The checklist of 5 early signs that shout colon cancer can help you decide.
One note for younger adults: colorectal cancer is rising in people under 50. Persistent rectal bleeding, ongoing abdominal pain, unexplained iron-deficiency anemia, or stool changes should not be brushed off because of age.
Screening is for people without symptoms. Diagnostic workup is what happens when something looks off. Mixing them up can cost time.
For average-risk adults, major U.S. guidelines recommend starting screening at age 45 and continuing through 75. Between 76 and 85, the decision is individual and depends on overall health and prior screening.
People with higher-risk histories often need earlier or more frequent screening.
If you have symptoms or an abnormal stool screening result, the next step is usually a diagnostic colonoscopy. Colonoscopy with biopsy is how colon cancer is confirmed, and blood tests alone cannot diagnose it.
Imaging and lab work help your team gauge how far the disease has reached. Common imaging includes computed tomography (CT) or positron emission tomography (PET).
Colonoscopy is typically performed by gastroenterology, and colorectal surgery by a surgical team. If a biopsy confirms cancer, our oncology team coordinates the next phase of care with those specialists.
Staging describes where the cancer is and where it has, or has not, traveled. It guides treatment choices and follow-up. Earlier stages usually mean more treatment options.
Stage 0 (carcinoma in situ): Abnormal cells sit only in the innermost lining of the colon. Nothing has grown deeper.
Stage I: Cancer has grown into deeper layers of the colon wall but has not reached lymph nodes or other organs.
Stage II: Cancer has grown through the colon wall and may have reached nearby tissue. It has not spread to lymph nodes, and it has not spread to distant organs.
Stage III: Cancer has spread to nearby lymph nodes. It has not yet spread to distant organs such as the liver or lungs.
Stage IV: Cancer has spread to distant organs or distant areas of the abdomen. The liver and lungs are the most common sites.
Your pathology report and imaging together tell the full story. The guide on everything you need to know about signs of colon cancer can help you ask better questions.
Treatment depends on stage, tumor features, your overall health, and what matters to you. Most plans use more than one tool, and the order they happen matters.
Surgery is the foundation for most stages. Very early cancers and some polyp-contained cancers can be removed during a colonoscopy.
More advanced disease typically requires removing the affected segment of the colon along with nearby lymph nodes. Healthy ends are usually reconnected, but a temporary or permanent colostomy is sometimes needed.
Colon surgery is performed by a colorectal surgeon, and we coordinate care with the surgical team.
Chemotherapy uses medicines that travel through the bloodstream to reach cancer cells. After surgery, it is often recommended for stage III to lower the chance of return.
Some higher-risk stage II cancers benefit too, though it is not routine for every stage II patient. Stage IV care often relies on systemic chemotherapy as a backbone.
Radiation therapy plays a smaller role in colon cancer than in rectal cancer. It can help in selected situations, such as treating a metastatic site or relieving symptoms. It is not a routine part of most colon-cancer plans.
Targeted therapy and immunotherapy can help some patients, but only when the tumor's biology fits. These treatments depend on biomarker testing, including mismatch repair (MMR) and microsatellite instability (MSI) status.
For tumors with MMR-deficient or MSI-high status, immunotherapy may become part of the plan. Other patients may benefit from targeted drugs based on different findings.
Many patients are not candidates, and standard chemotherapy is often the better-supported option in those cases.
At ACTC in Brooksville, our medical oncology, radiation oncology, and hematology oncology teams work together under one roof. Treatment delivery on site includes:
Chemotherapy infusion
Immunotherapy and targeted therapy when biomarker testing supports them
Imaging with in-house computed tomography and mobile positron emission tomography
A full on-site lab
Financial counseling is available for the practical side.
Colonoscopy, colorectal surgery, genetic counseling, and ostomy care are typically handled by partner specialists, and we coordinate alongside them. You can review the broader scope of colorectal cancer treatment we coordinate. We also support patients with related diagnoses, including stomach cancer treatment.
A colon cancer diagnosis brings travel, scheduling, and decision fatigue at the worst possible time. Care close to home takes some pressure off. Our 21,000 square foot center on Cortez Boulevard serves patients in Brooksville, Spring Hill, Weeki Wachee, and across Hernando County.
Medical oncology, radiation oncology, hematology oncology, and supportive imaging are all on site. Bringing imaging discs, pathology reports, and written questions to the first visit helps our team move quickly on a plan.
It depends on where the cancer starts. Colon cancer begins specifically in the colon. Colorectal cancer is the broader term covering cancers that start in the colon or rectum, both part of the large intestine.
Not necessarily. Early colon cancer often causes no symptoms, which is why screening at 45 matters even when you feel fine. When symptoms do appear, they tend to be persistent changes such as rectal bleeding, bowel-habit changes, abdominal pain, fatigue, or unexplained weight loss.
Start with 45 if you are at average risk. Major U.S. guidelines recommend continuing through 75, with individualized decisions between 76 and 85.
People with inflammatory bowel disease, certain polyp histories, or strong family risk often start earlier.
Staging describes how far the cancer has grown or spread. Stage 0 and stage I cancers are usually treated with surgery alone. Stage II often involves surgery, with chemotherapy considered for higher-risk pathology.
Stage III typically pairs surgery with chemotherapy. Stage IV is usually managed with systemic therapy, and in selected cases surgery or radiation aimed at specific sites.
It depends on the stage and risk features in your pathology. Many people with stage 0 or stage I do not need chemotherapy after surgery. Some higher-risk stage II cases benefit, while many do not.
Most stage III patients are offered chemotherapy after surgery. Most stage IV plans include systemic therapy.
Sometimes. These treatments depend on biomarker results from the tumor, including MMR and MSI status. For tumors with MMR-deficient or MSI-high status, immunotherapy may help, but many patients are not candidates.
A colon cancer diagnosis raises more questions than one appointment can answer. You do not have to sort it out alone. Our team in Brooksville can review your pathology, imaging, and questions.
We will map out next steps with you. Call 352-345-4565 or book a visit at https://actchealth.com/appointment.


January 07, 2026
A chemo port is a small device placed under your skin that makes recei...
KNOW MORE
December 24, 2025
It's natural to wonder if testosterone replacement therapy (TRT) is sa...
KNOW MORE
December 24, 2025
A rash that will not calm down is scary, especially when it changes or...
KNOW MORE
December 24, 2025
Florida’s lung cancer burden remains significant and affects many fa...
KNOW MORE
December 24, 2025
A partial hysterectomy, also called a supracervical hysterectomy, is s...
KNOW MORE
December 24, 2025
Finding a rash on your breast can be unsettling, but remember, many ra...
KNOW MORE
