
Book a Consultation
Thank you!
Your form has been sent successfully.



March 25, 2021
The pancreas is an important digestive and endocrine organ located within the abdomen behind the stomach. The pancreas is responsible for the production of insulin, the primary hormone responsible for glucose transport in humans. Pancreatic cancer is a deadly form of cancer that occurs when the cells of the pancreas grow rapidly and form a malignant mass of tissue, causing a host of debilitating health problems.
There are two major sub-types of pancreatic cancer named for the cells in which they originate:
Exocrine pancreatic cancer affects the tissues that produce, carry, and secrete digestive enzymes.
By far the most common type of exocrine cancer is pancreatic ductal adenocarcinoma (PDAC), representing approximately 85% of cases. The majority of these growths occur in the epithelium of the pancreatic ducts, a system of vessels that carry enzymes and other secretions away from the pancreas.
Common symptoms of PDAC include non-specific symptoms like abdominal pain and swelling, vomiting, nausea, jaundice (yellowing of the skin and eyes), intestinal bleeding, anemia, and fatigue.
The second most common type of pancreatic cancer is acinar cell carcinoma. ACC represents approximately 2% of cases in adults and roughly 15% in children. This pancreatic cancer sub-type begins in the cells that produce digestive enzymes of the pancreas.
ACC may cause many of the same symptoms as PDAC, such as pain, fatigue, and nausea. Jaundice is uncommon in cases of acinar cell carcinoma.
The survival rate for exocrine pancreatic cancer is abysmally low. 34% of local non-invasive cases, 12% of regional invasive cases, 3% of distant metastatic cases, and 9% across all stages will survive exocrine pancreatic cancer over 5 years. This is mostly in part because pancreatic cancer is often diagnosed after it is too late to perform surgery to remove the malignancy.
Endocrine pancreatic cancer is a rare form of pancreatic cancer that affects the tissues that integrate the nervous and endocrine systems of the body within the pancreas. Endocrine pancreatic cancer presents as pancreatic neuroendocrine tumors (PNETs) or islet cell tumors, denoting the specific type of cells they grow from.
PNET growths are categorized as functional and non-functional tumors depending on whether or not they secrete excess hormones.
Functional PNET symptoms and classifications vary depending on the type of hormones they secrete:
Gastrinoma cause acid reflux, abdominal pain, diarrhea, weight loss, and fatty stool. Glucagonoma causes high blood sugar, severe irritation of the skin, sores of the mouth, anemia and weight loss.
Insulinoma causes low blood sugar, shakiness, and confusion.
Somatostatinoma causes the suppression of a variety of hormones resulting in non-specific symptoms including diabetes, weight loss, gall stones, fatty stool, diarrhea, nausea, and vomiting. Vasoactive intestinal peptide releasing tumors (VIPoma) cause diarrhea, muscle weakness, nausea, and fatigue.
The 5-year survival rate for endocrine cancer is quite high at around 92% for localized non-invasive cases, 76% for regional invasive cases, and 27% for distant metastatic cases. The average survival rate across all stages is roughly 55%, which is comparatively much higher than the survival rate for cases of exocrine pancreatic cancer.
About 25% of pancreatic cancer cases can be attributed to tobacco use, making it the leading preventable cause. That includes smokeless tobacco, cigars, and cigarettes, so your best bet is to quit tobacco now to lower your risk.
Obesity is another major preventative risk factor; obese people are 20% more likely to develop pancreatic cancer than non-obese people. Type II diabetes (another risk factor associated with pancreatic cancer) is also common among obese people; it’s unclear whether or not people with juvenile (type I) diabetes face a greater risk of developing pancreatic cancer.
Strategies that involve diet modification in concert with regular physical activity are the most effective at lowering body mass index and reducing your risk of diabetes as well as most types of cancer. You can find recommendations on exercise and nutrition for cancer prevention here.
About 10% of pancreatic cancer cases can be attributed to a genetic component. Genetic mutations resulting in conditions such as Peutz-Jhegers syndrome and Lynch syndrome may cause cancerous and pre-cancerous lesions throughout the digestive tract, markedly increasing the risk of developing pancreatic cancer.


January 07, 2026
A chemo port is a small device placed under your skin that makes recei...
KNOW MORE
December 24, 2025
It's natural to wonder if testosterone replacement therapy (TRT) is sa...
KNOW MORE
December 24, 2025
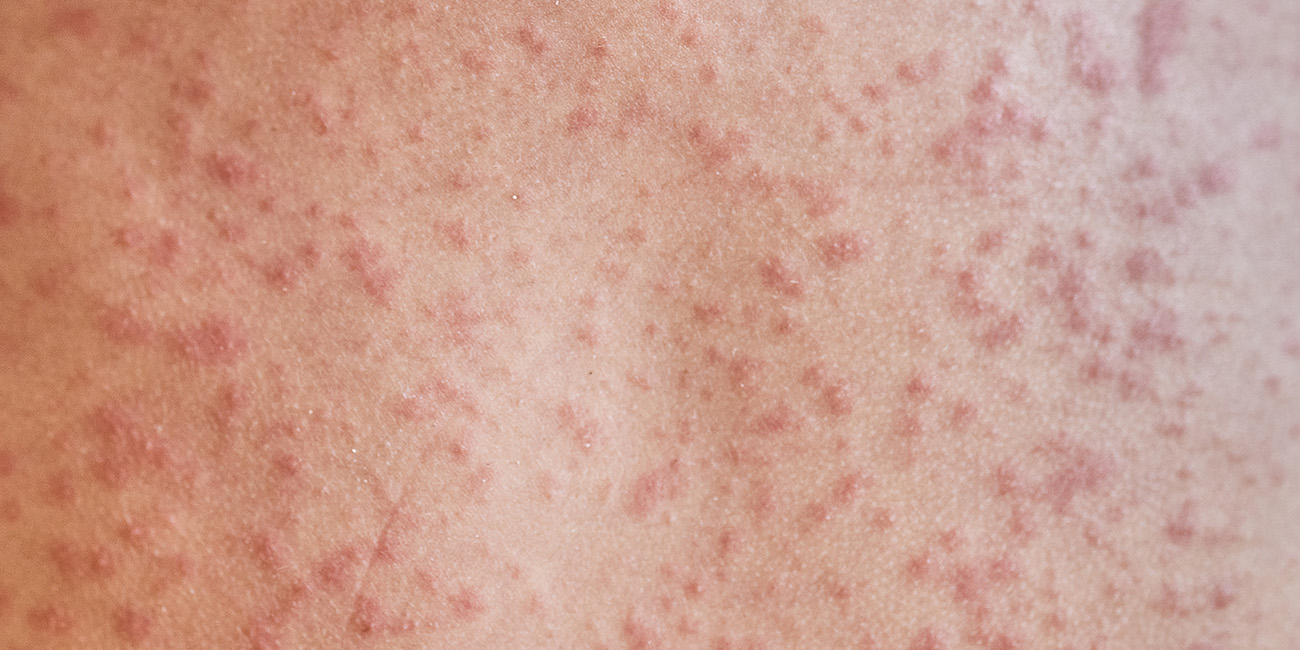
A rash that will not calm down is scary, especially when it changes or...
KNOW MORE
December 24, 2025
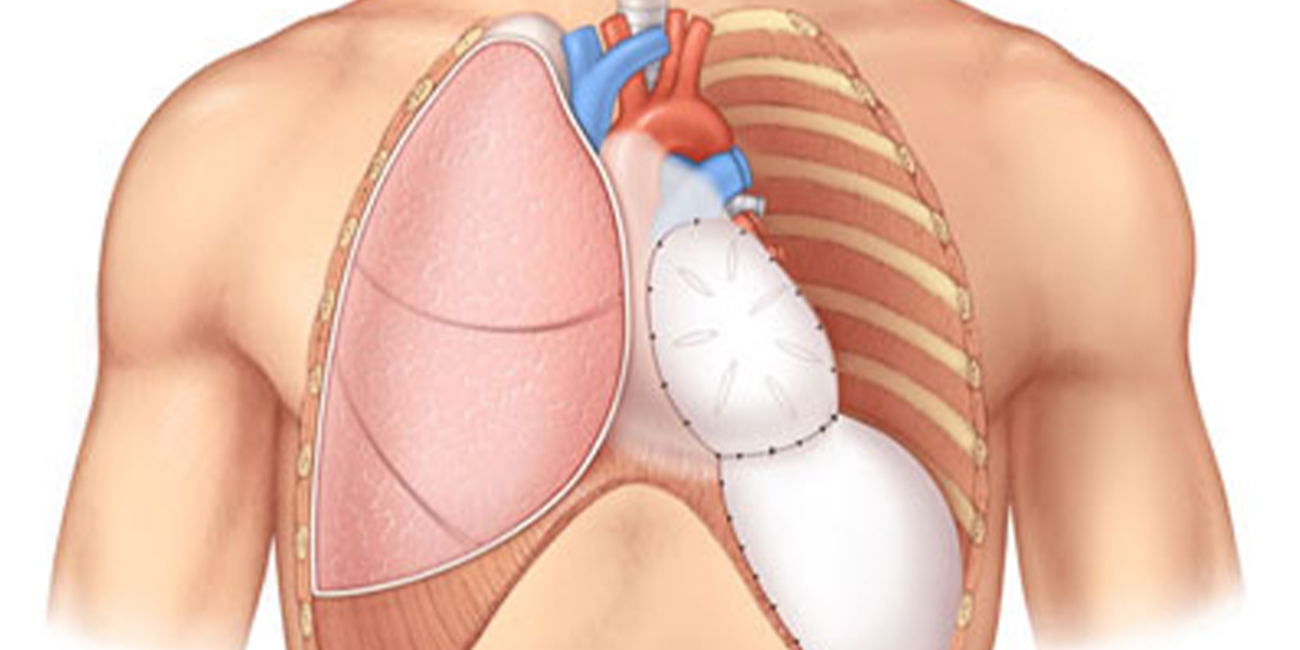
Florida’s lung cancer burden remains significant and affects many fa...
KNOW MORE
December 24, 2025
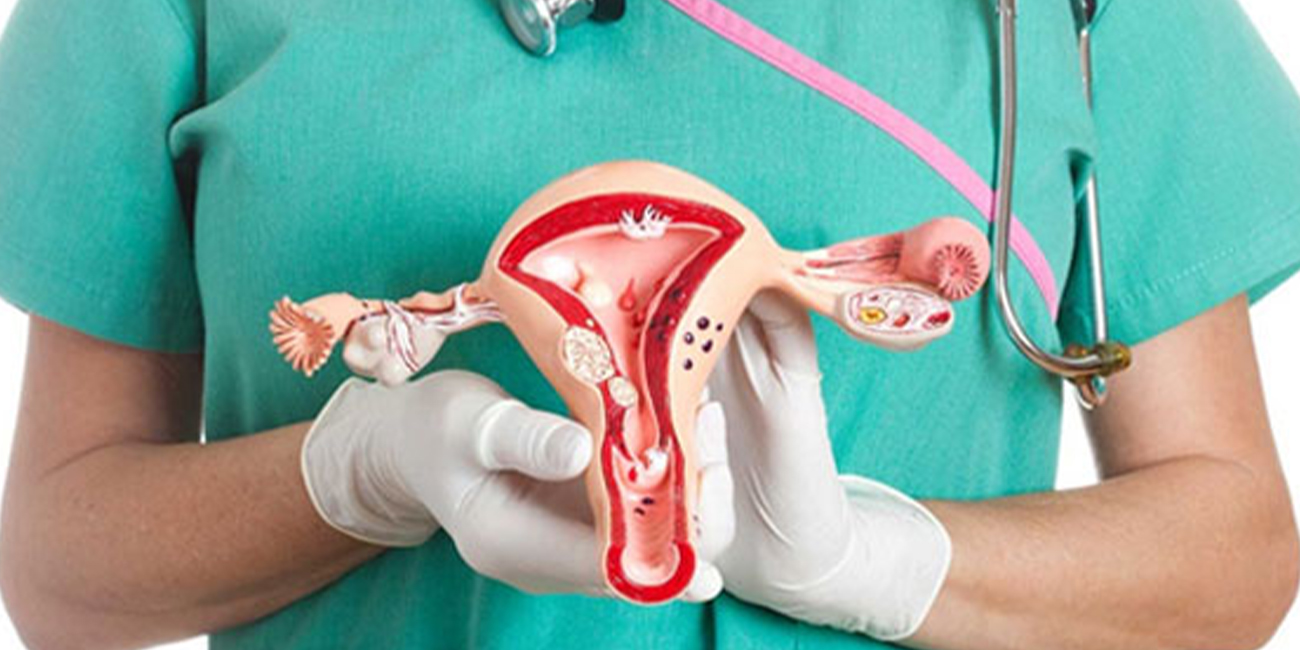
A partial hysterectomy, also called a supracervical hysterectomy, is s...
KNOW MORE
December 24, 2025
Finding a rash on your breast can be unsettling, but remember, many ra...
KNOW MORE
