
Book a Consultation
Thank you!
Your form has been sent successfully.


May 27, 2021
Testicular cancer is among the most curable cancers today. Still, it is that one disease that the average male prefers not to have a conversation about, even though talking about it could save lives.
Compared to other kinds of cancer, the cure rate for testicular cancer is excellent. Treatment for testicular cancer is fast, effective, and its cure rate is notably high. However, patient response to the treatment completely depends on the cancer cell type, its spread, and the patient?s overall health. In the course of their lifetime, 1 in 270 US men are estimated to get diagnosed with testicular cancer as per the report by Johns Hopkins and the mortality rate due to it is very low (even less than 1 in 5000 US men).
Testicular cancer is a type of cancer that originates in one or both male organs known as testicles or testis.Testicular cancer commonly starts with mutations in the germ cells.
Testicular cancer is rare, but it can affect a full-grown male or boy at any age. It is usually found in men between the ages of 15 to 44 years (average age of diagnosis of 33 years old). Men with a physical disorder of the testicles (at any age) might have a higher risk. It is also noted that in the US, white men are more prone to testicular cancer than African-American men.
Treatment for testicular cancer is determined on the basis of the type of cancer and the prognosis of an individual. Testicular cancer can occur in the hormones producing tissues, and these tumors are classified as gonadal stromal tumors. Apart from this, the most common kind of testicular cancer is germ cell testicular cancer. The two primary types of germ cell testicular cancers are:
Seminomas have become very common in the past 20 years and now account for more than 40 to 45% of testicular cancers. This type of testicular cancer is caused by a young germ cell that stays relatively immobile and grows slowly. Seminomas are normally restricted to the testes, but in some cases, lymph nodes may also be involved.
Non-seminoma is the more common form of testicular cancer than seminoma. This type of testicular cancer is faster growing which emerges from more mature germ cells and may even spread to other parts of the body. Non-seminomas account for most of the choriocarcinomas, embryonal carcinomas, and yolk sac tumors. Non-seminoma tumors tend to be more aggressive.

Most of the lumps in the scrotum are not always cancerous, but it is necessary to get examined as soon as possible. Treatment for testicular cancer is highly effective when diagnosed in an early stage. The tests and screenings a specialist generally uses to diagnose testicular cancer at cancer treatment centers include:
Markers in your blood that are linked to specific types of cancers may include:
During the physical examination, the doctor looks for testicular abnormalities, like lumps or swelling that might be associated with testicular cancer.
The ultrasound scan is a painless procedure that helps your specialist with determining the location and spread of the tumor inside of your testicle. This technique uses high-frequency sound waves and produces an inside image of a testicle. It is one of the main methods that give a clear indication of the location and type of the tumor or lump.
To confirm a diagnosis, a series of blood tests are done to identify and measure the amounts of certain hormones (known as markers) present in the blood. These tests are also known as tumor marker tests and show raised levels of blood hormones related to testicular cancer.
These tests and reports are the only definitive way to confirm testicular cancer.
Note: Some individuals with testicular cancer may not produce markers. Thus, there may be a possibility of testicular cancer even if the blood test results are normal.
After the completion of all screenings and tests, it is generally possible to discover the stage of cancer. Testicular cancer is usually categorized based on the response to treatment. It can be good to intermediate and poor. The testicular cancer stages are noted by Roman numerals ranging from 0 to III. Three stages of testicular cancer are:
In this stage, cancer is limited to the testicle and epididymis. Apart from this, all tumor marker levels are tested normal.
This stage refers to patients with cancer spread to the lymph nodes in the back of the abdomen, but not anywhere else.
Stage III cancer is determined when cancer has spread to other parts of the body. This type of cancer is considered advanced and usually spreads to the lungs, liver, brain, and bone.
After the diagnosis, you may have questions and doubts about your possible treatment options. Your healthcare provider will explain about possible treatment choices you have, how they are expected to work, and the risks and side effects associated with it. You may be advised of one or more specific treatments.
The possibilities and process for treating testicular cancer depend on various factors like the type and stage of cancer, the overall health, and the preferences of a patient. Sometimes recommended treatment plans depend on the type of cancer because seminomas are sensitive to radiation, and both seminoma and non-seminoma tumors are sensitive to chemotherapy.
If a testicular tumor is detected with both seminoma and non-seminoma cells, it is treated as a non-seminoma. The three major treatments for testicular cancer are:
Surgery is the prime procedure for approximately all stages and kinds of testicular cancer. Surgical operations practiced to treat testicular cancer involve:
Surgery to remove your testicle:In this procedure, the surgeon makes an incision in the groin and extricates the complete testicle. In some cases of early-stage testicular cancer, just the surgical removal of testicles may be the only treatment required. Despite this surgery, you will be required to follow surveillance procedures and have regular check-ups and screenings to make sure that cancer hasn?t returned.
Surgery to remove lymph nodes: Sometimes, the removal of testicles is not enough, and the removal of lymph nodes must be performed. This procedure is performed through an incision in your abdomen, and the surrounding lymph nodes are removed. In medical terms, this surgery is known as Retroperitoneal Lymph Node Dissection (RPLND).
In radiation therapy, high-energy rays are used to destroy cancer cells. If cancer cells have spread into the lymph nodes, the patient may need to go for radiotherapy after chemotherapy. Radiation therapy is usually successful in treating seminomas. It can be administered in two ways, externally as well as internally at the cancerous area.
External: External therapy uses high-energy radiation beams directly at cancer cells to destroy them.
Internal: Internal Radiation therapy comprises a radioactive substance in catheters (thin flexible tubes) or needles placed into the cancer cells or right next to them.
Side effects of radiotherapy involve nausea, fatigue, redness of the skin, and irritation in abdominal and groin areas. Radiation therapy may also reduce sperm counts temporarily, but it gets better with time.
Chemotherapy is a systemic treatment that uses medication to destroy cancer cells by traveling through your bloodstream. Drugs used in chemotherapy also destroy cancer cells that may have transferred to the other body parts from the original tumor. Chemotherapy can be taken both orally and through the veins.
Many specialists prefer to use chemotherapy over radiation therapy because it appears to be easier to tolerate. In some advanced cases, high-dose chemotherapy may be used to destroy the cancer cells.
Side effects of chemotherapy depend on the drugs used for the treatment, but some common side effects are fatigue, nausea, and hair loss. These side effects are not permanent, and some medications are available to reduce the side effects of chemotherapy.
Stem Cell Transplant is not very common, but if your cancer treatment needs higher doses of chemotherapy, it can help your body handle it.
Stem cell transplant helps in replacing cells that are destroyed during cancer treatment.Stem cells in this treatment are taken from the patient?s own blood or bone marrow. The stored frozen stem cells are liquefied and returned back to the patient?s body through the infusion process.

Researchers are always on to finding new testicular cancer treatments. These methods are tested in clinical trials. Being a part of clinical trials means getting the best treatment available, and one might also get treatments that are considered to be even more beneficial. Before starting with your treatment, discuss with your healthcare provider and find out about available clinical trials.
Although testicular cancer is a treatable cancer, there is still a possibility of it spreading to other body parts. Removing testicles may help you get rid of cancer but can affect your fertility too.At ACTC Health, we use novel procedures to treat testicular cancer. Our treatment program is created by oncologists specialists who make sure that every patient gets personalized cancer care at every step of their treatment. This approach helps us deliver the best possible results, and if any other treatment modifications are required, our oncologists recommend evidence-based therapies and options.
Infographic



January 07, 2026
A chemo port is a small device placed under your skin that makes recei...
KNOW MORE
December 24, 2025
It's natural to wonder if testosterone replacement therapy (TRT) is sa...
KNOW MORE
December 24, 2025
A rash that will not calm down is scary, especially when it changes or...
KNOW MORE
December 24, 2025
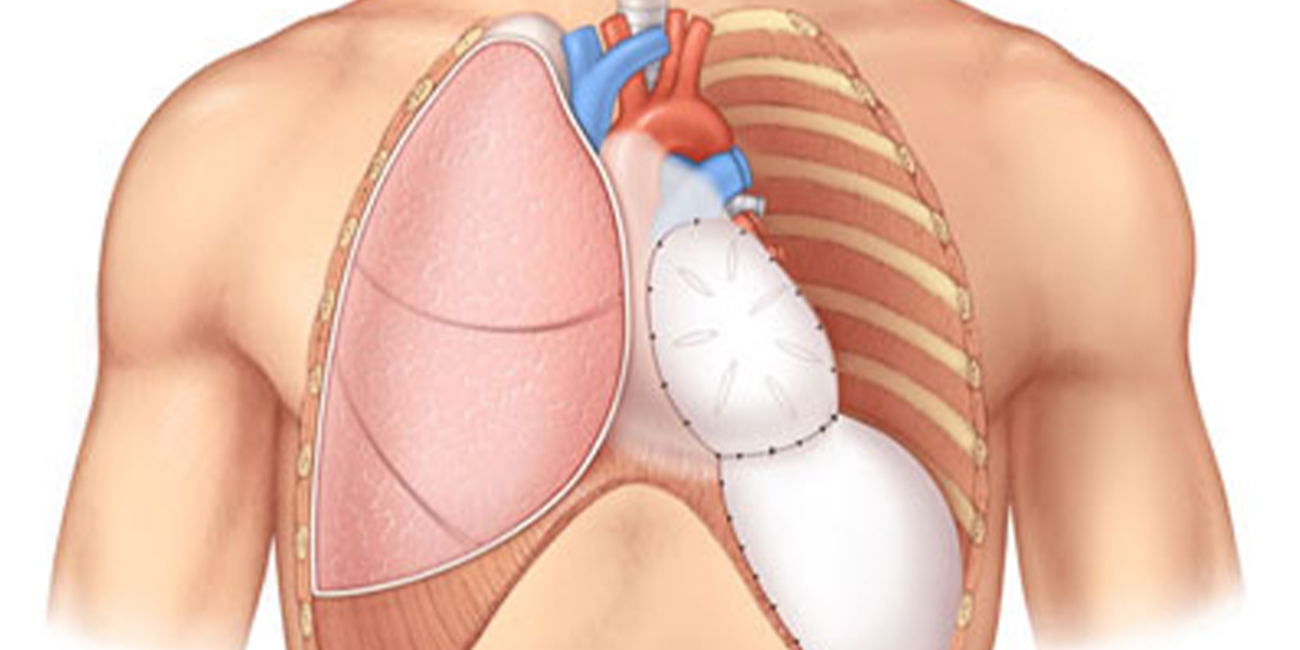
Florida’s lung cancer burden remains significant and affects many fa...
KNOW MORE
December 24, 2025
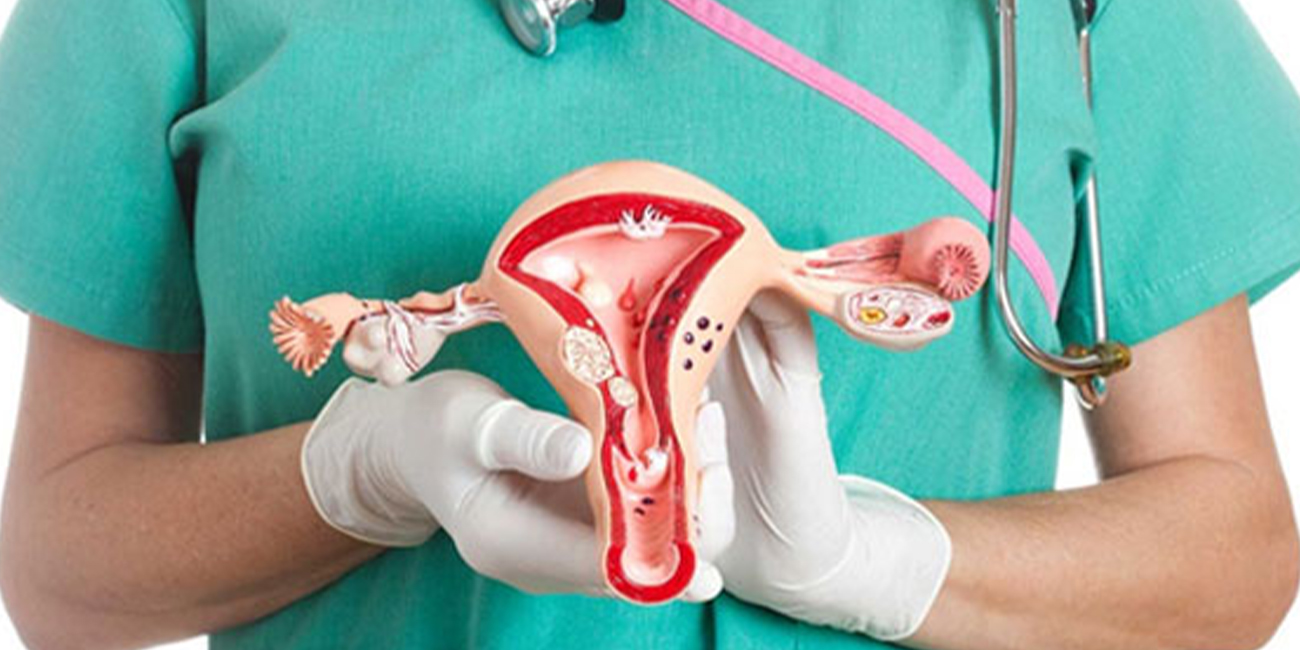
A partial hysterectomy, also called a supracervical hysterectomy, is s...
KNOW MORE
December 24, 2025
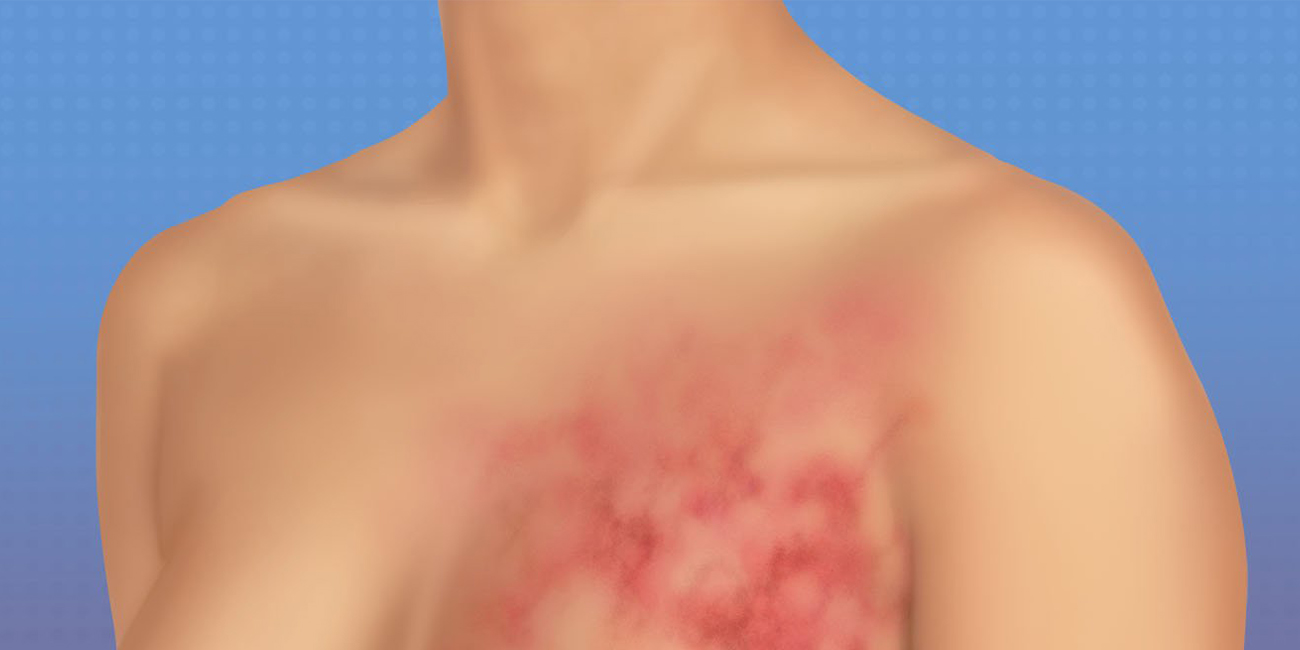
Finding a rash on your breast can be unsettling, but remember, many ra...
KNOW MORE
